HHS’ ICD-10 Code Deadline Arrives
With the arrival of October 2015 come changes beyond the color of the leaves, as it signifies the U.S. Department of Health and Human Services’ (HHS) deadline for hospitals, physician practices, other healthcare providers and payers to have completed the transition from ICD-9 to ICD-10 (International Classification of Diseases, Revision 10) coding systems. ICD-10 provides more granular coding during a patient’s medical treatment, generating specific data that is expected to improve healthcare delivery. Benefits of the more advanced coding include the ability to:
- Develop a more detailed patient history
- Better coordinate patient care across providers and over time
- Improve quality measurement and reporting
- Detect and prevent fraud, waste, and abuse
- Gain more accurate metrics for Federal or private insurance reimbursement
Additionally, since ICD-10 coding includes more complete information on the medical conditions that providers treat, the level of data capture and analytics is expected to allow for more advanced surveillance of public health and quality reporting on a national scope.
For all of these benefits of implementing a more complete medical coding system, it has been a process fraught with difficulties…particularly for healthcare providers and insurers. They have had to shoulder most of the financial responsibility for the operational upgrades necessary to be able to track, code, store and share the data-heavy ICD-10 coding system that is required to participate in reimbursement programs.
Porter Research – a Billian Company – has been working with many healthcare organizations over the past few years leading up to the ICD-10 deadline to develop research programs that would provide key metrics of what was taking place in the healthcare marketplace, as providers scrambled to fund and implement these changes within their business model to achieve regulatory compliance.
“I recently attended the AHIMA [American Health Information Management Association]trade show, and there was a lot of optimism going around about the kickoff for ICD-10, and how well things were going,” said Cynthia Porter, president of Porter Research. “But there’s also the lingering question about what happens if claims don’t get paid in 30 days-time. I think there is an undercurrent of nervousness about the potential for claims to be denied for some unexpected reason. In the end, only paid claims will start alleviating the concerns held by healthcare providers and payers. Training and workflow challenges associated with the ICD-10 transition will continue well past October.”
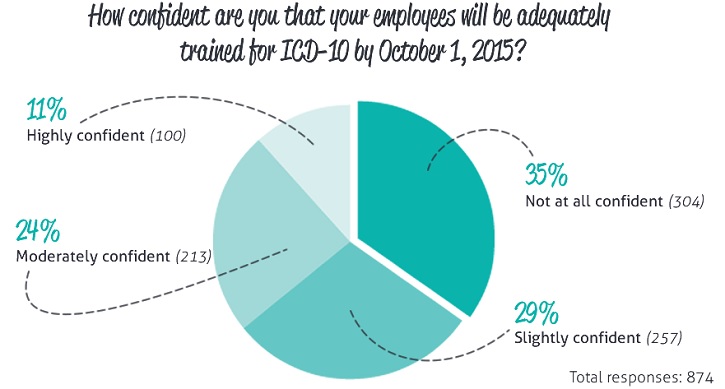
Navicure, a provider of cloud-based healthcare billing and payment solutions, commissioned Porter Research to conduct a recent national survey of healthcare organizations to gauge their preparedness for the ICD-10 transition. The August 2015 Healthcare Organization ICD-10 Readiness Survey revealed a mixture of confidence along with apprehension from survey participants, the majority (58%) of whom serve as physician practice administrators or billing managers. Some key survey findings include:
- 85% of respondents stated that they are optimistic about ICD-10 preparedness
- 94% of respondents anticipate an increase in their claims denial rate
- Over 50% of respondents anticipate a negative impact on their organization’s finances, operations and staff morale as a result of the transition to ICD-10.
“The ICD-10 Readiness Survey that Porter Research conducted helped Navicure understand what was important and needed in the marketplace to meet the HHS deadline. This insight from key healthcare industry stakeholders allows Navicure to better understand the market realities of what is actually taking place during the transition,” stated Phil Dolan, Navicure’s Chief Marketing Officer. “Thankfully, it appears that the ICD-10 deadline arrival has been uneventful so far, as we enter into October. I think this level of preparedness indicates how hard providers and vendors have worked together over the past few years in order to reach this point.” To view the complete survey key findings and action items, visit survey results
Navicure has been working with healthcare providers to assist them through the ICD-10 transition process, to ensure that their day-to-day business operations avoid unnecessary disruption. The IT solution company even offers free access to ICD-10 transition tools that include online correction of rejected claims, expanded claim tracking, and ICD-9 to -10 mapping for any payers that turn out to be unprepared for the change. Navicure’s ICD-10 resource webpage is available at click here
The Centers for Medicare & Medicaid Services (CMS) announced earlier this year that non-compliant ICD-10 Medicare claims would be accepted during the 12-month period past the deadline date. However, this does not extend to Medicaid, BCBS and commercial plans. Additionally, the CMS is working with the American Medical Association (AMA) on a series of proactive initiatives [ For more details, click initiative ] to help physicians and other healthcare providers that are struggling to achieve regulatory compliance. The two agencies – representing governance and the medical community – realize the need for addressing the individual challenges faced by healthcare providers beyond an inflexible deadline date as the healthcare industry modernizes its coding system nationwide.